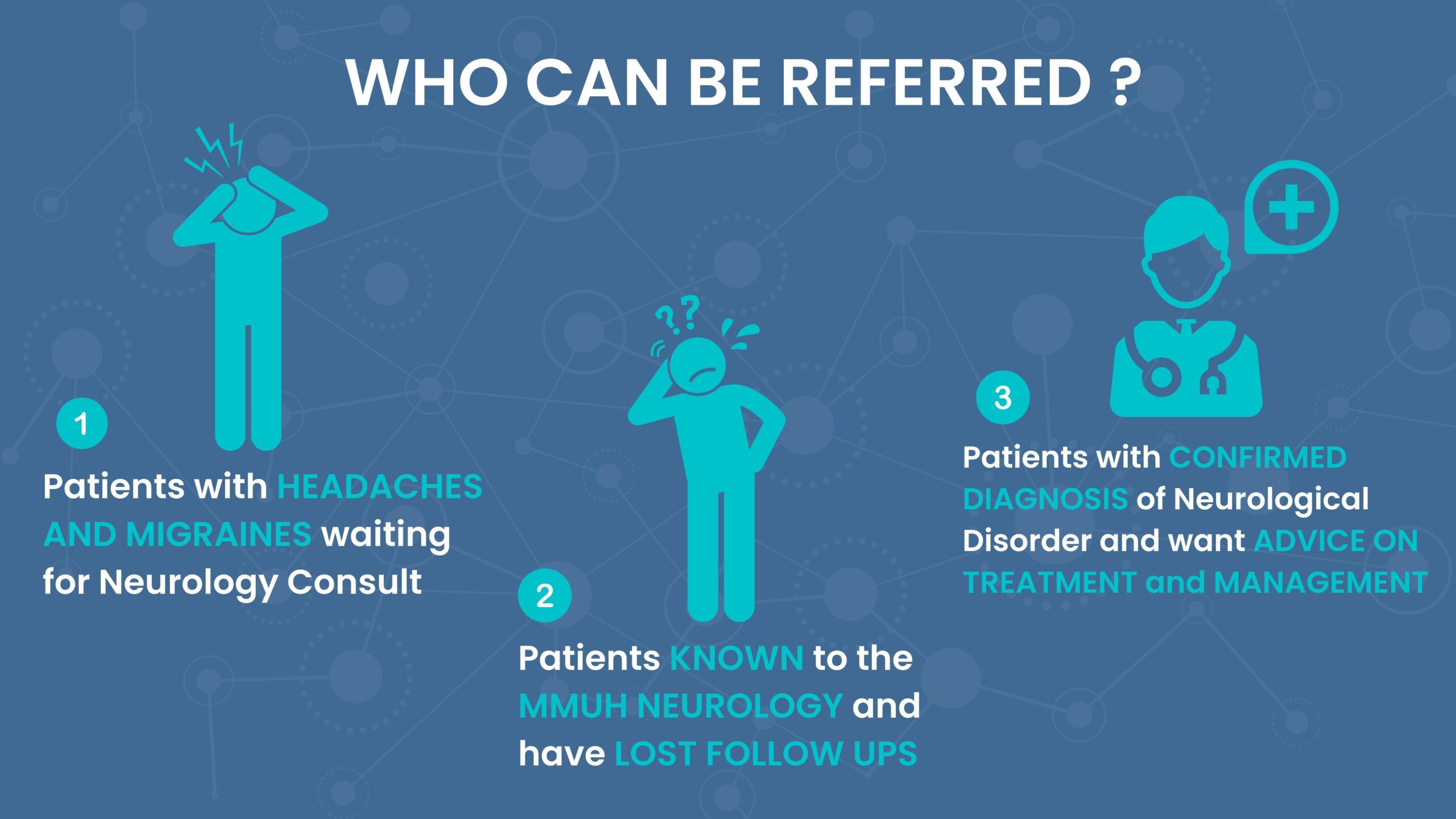
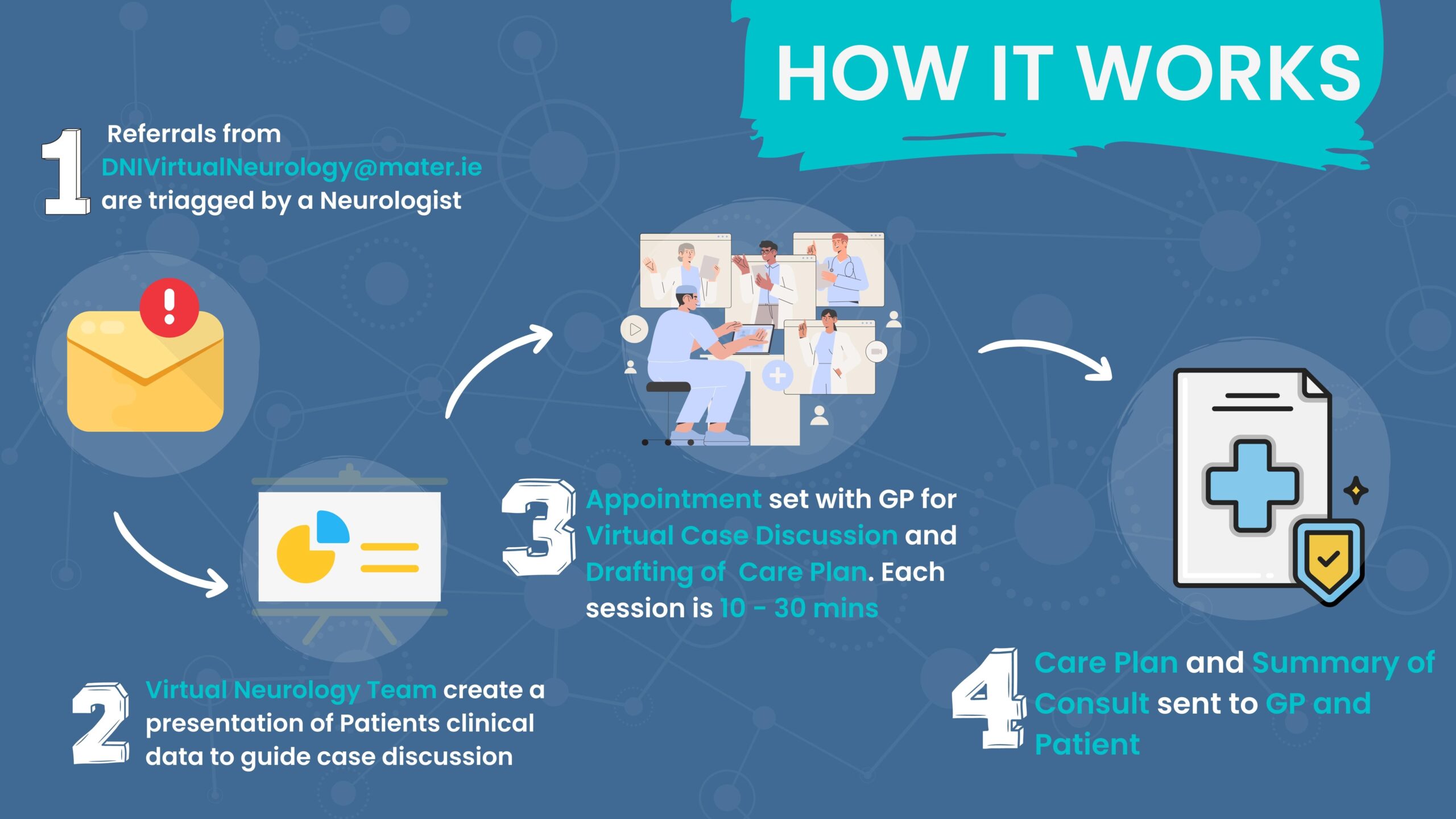
Neurology Virtual Consultation Clinics Pilot Project
The Dublin Neurological Institute, in partnership with HSE Community Health Organization for Area 9, is piloting a new service for GP practices to improve health outcomes of neurology patients in the community. This service is currently being piloted in several areas within the CHO Area 9.